Do You Need Milk For Strong Bones? Marketing Says Yes But Science Says No.
“Milk helps build strong bones and teeth!”
Like many, I first heard this mantra when I was a child in elementary school and it is a message that is firmly ingrained in the minds of most as one of the few universal truths in nutrition. The need for dairy products as an irreplaceable part of the human diet for building and maintaining strong bones and warding off the ravages of osteoporosis is considered common knowledge, an unshakable truth, and a message repeated ad nauseum in the media. A message that few would find reason to question. It’s no secret that milk contains calcium- a key mineral for maintaining bone health. Thus, there would appear to be little reason to question its importance as a protective shield against bone loss. As popular and seemingly rational an idea as it may be, the scientific evidence doesn’t support it. Very early in my career I myself was quite surprised to learn that my early indoctrination to the health benefits of dairy consumption didn’t come from credible peer reviewed scientific research, but from a rather successful marketing campaign on the part of the dairy industry. A campaign influential enough to have the US government (and many others around the world) classify milk as a food group- a decision made based on profit and not sound nutritional science. Contrary to popular belief billions of people on the planet do just fine without having milk as a part of their diet. Not hundreds of thousands or millions, but billions. Surprisingly enough, people in countries where milk consumption is minimal have some of the lowest incidences of osteoporosis and hip fractures on earth. A revealing statistic that somehow never seems to find its way to American audiences, nor does the fact that for hundreds of thousands of years, most humans on the planet didn’t drink milk and that many enjoy rather robust health without it. There is a reason for our rather myopic understanding of milk and what it can and cannot do for us and it’s the dairy industry. The reach of the dairy industry’s influence is impressive to say the least, spreading information designed to help them sell more milk not just nationally but globally.
Using a consumer creating model sanctioned by government entities, teaching material for young children in schools about the role of milk in building strong bones and teeth is graciously supplied by the American Dairy Council. Presented as educational material at an early age, such influence affects our perception of milk as a required part of our diets and it is hard, if not impossible for a child to question such authoritative information. An effective model that ensures that as adults the party line that milk is a requirement for optimal health is firmly rooted in our core set of beliefs. It’s a similar methodology used by fast food chains like McDonald’s to market to children, knowing fully well that it will guarantee another generation of customers.

Not only is milk taught at an early age to be an essential part of our diet, it is provided to us as well. As a food product produced far in excess of what we as a nation can consume thanks to heavy government subsidies secured by the dairy lobbies, it can be literally given away and dairy producers still make profits. With the early consumer marketing model in mind it thus makes sense that milk is distributed to young children in schools through government food programs. Good business as it helps to cement the thought process of milk being a necessity as an unquestioned view.
Milk & Calcium- Understanding The Science

As adults we are bombarded by messages and dairy lobby funded ‘studies’ reminding us about the calcium content of milk and dairy products. Most notably for women and the steadily aging American population, milk’s supposed prophylactic effects against bone loss are emphasized. But can the calcium in milk really make a difference in bone density? Looking internationally at the dairy-equals-calcium-which-equals-strong-bones idea, we see clearly that the countries with the highest rates of osteoporosis are the largest consumers of dairy products. The dairy consumption of countries like the United States, Australia, New Zealand, Switzerland, the UK and Northern Europe is enormous when compared to Asian countries such as China where dairy consumption is rare, yet those very countries where less dairy is consumed have they have the lowest rates of hip fracture and osteoporosis in the world.[1,2,3,4]
Rates Of Osteoporosis Are Lower In Populations Who Do Not Consume Milk & Dairy Products
To give an idea of the prevalence of osteoporosis, estimates are that 40% of American Caucasian women and 13% of Caucasian men aged 50 years will experience at least one bone loss related fracture in their lifetime. At age 50, a Caucasian woman has a 17% chance of sustaining a hip fracture, 15% chance of vertebral fracture and 16% chance for forearm fracture, with comparable figures of 6%, 5% and 2.5%, respectively, for fractures in white males.[2] Interestingly enough among the female African American population the age-adjusted prevalence of hip related osteoporosis is only 6%, compared to 17 % for postmenopausal White women- difference consistent with the much lower fracture rates observed in African Americans.[5] African Americans, by the way consume almost 40% less milk and dairy products as their Caucasian counterparts[6] which if by itself renders the milk/dairy-equals-strong-bones theory to be questionable. Statistics from the observation of low dairy intake in Asian population contradict the milk/dairy-equals-strong-bones theory completely. Using China as an example, where cheese and other popular dairy products are not a part of their regular diet and where milk consumption is 10% of the American per capita consumption rate [7] age standardized incidence of hip fractures is far lower than their milk drinking American and European counterparts. Based on the 1990 China census figures hip fracture rates were only 87 per 100,000 for women and 97 per 100,000 for men. Contrast these numbers with 510-559 per 100,000 for white American women and 174-207 per 100,000 for American Caucasian men[8]. In fact, hip fractures in Beijing are reportedly among the lowest rates of occurrence in the world- and with a population where milk is by no means a staple.
Debunking The Need for Milk- It’s The Calcium Lost Not Calcium Consumed That Causes Osteoporosis
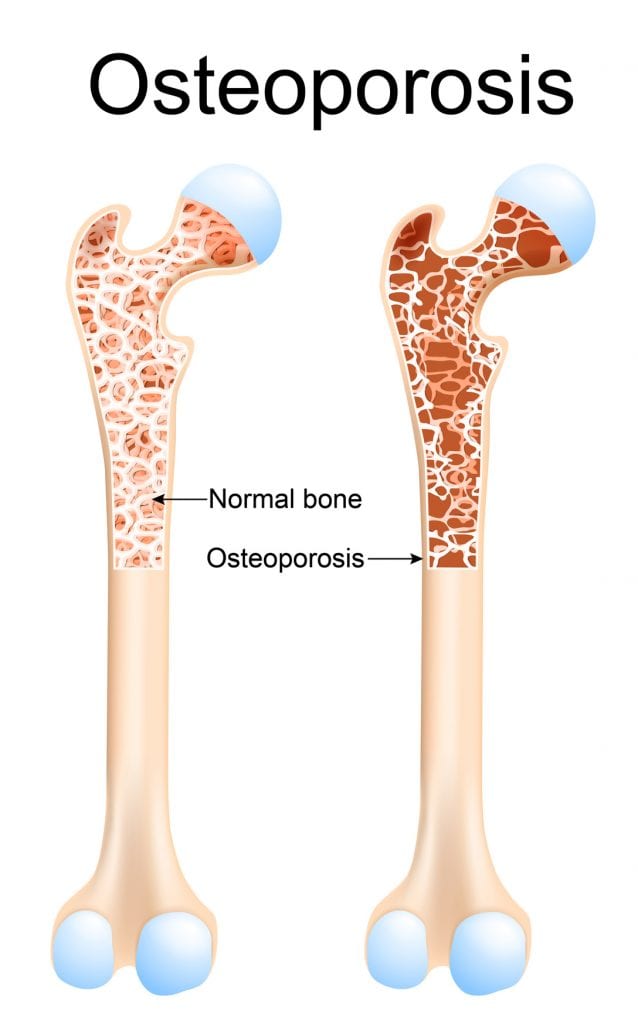
As much as the good (and well paid) folks at the American Dairy Association would like you to think that increasing your calcium intake by drinking milk would decrease your risk of osteoporosis, the science behind this premise simply doesn’t support it. From what we do know about bone loss, it happens not so much from not having a high enough calcium intake, but rather from having a high level of calcium loss due to dietary and lifestyle choices. [8] According to the findings of the 1994 National Institutes of Health Consensus Conference, at least one third of calcium balance and bone density is dependent on the ratio of intake to loss and not solely on calcium intake alone as the marketing campaigns would have you believe. To be frank, meta-analysis of literature meeting the provisions for unbiased scientific research found there were no significant relationships proved between milk consumption or any other dairy product to measures of bone health nor were there no correlations between calcium intake and bone loss.[9,10,11,12] Similarly, an 18 year analysis of 72 337 postmenopausal women published in the February 2003 American Journal of Clinical Nutrition, found that an adequate vitamin D intake was associated with a lower risk of osteoporotic hip fractures in postmenopausal women. Neither milk nor a high-calcium diet in the study had any correlation with a reduction in risk of osteoporosis.
Milk Isn’t The Best Or Only Source Of Calcium

So we have established that bone loss has little to do with intake, but for those concerned nevertheless about their calcium intake, it should be noted that a 1990 report in the American Journal of Clinical Nutrition found that green leafy vegetables such as broccoli and kale have high levels of calcium and is absorbed at least as well as the calcium in milk. [12,13,14] Proper calcium balance on a non-dairy diet is easily attained because ALL vegetables and legumes contain calcium. [15] Thus within the context of a balanced diet it is more than adequate to prevent frank deficiencies which are rare to nonexistent in developed countries such as the United States.[16] In terms of the ultimate source of calcium, however no other food source can compete with the bioavailability of calcium from bones. That’s right, bones. You don’t hear much about it since eating bones isn’t that popular here in the United States and given that both dairy producers and supplement manufacturers would be hard pressed to sell their wares if the general population was aware that eating small amounts of bone is how humans got most of their calcium for several hundred thousand years. The small and soft bones of fishes like sardines are a perfect source of calcium in a form our bodies can easily absorb, as is the use of bone meal that can be added to soups and broths. Since these sources are better absorbed (and it makes sense that bones would be the best source of building material for bones) our body retains more of it as opposed to being mostly excreted in urine as is often the case with dairy products and artificial supplements.
Osteoporosis is a very real concern for many women, as they make up 80% of those affected by this condition. Osteoporosis is a major public health threat for an estimated 44 million people here in the United States with almost 10 million individuals estimated to already have the disease and almost 34 million more are estimated to have low bone mass, placing them at increased risk for osteoporosis. It is time we paid more attention to what has been proven to be real risk factors, such as soda consumption, high sodium diets, smoking, excessive caffeine consumption, alcohol and an inactive lifestyle, than simply falling for the marketing hype that somehow drinking milk or eating yogurt and cheese will magically protect you from low bone density.
Getting the recommended daily allowance of calcium at all ages is important, preferably from dietary sources. But bone nutrient requirements are wide and far more complex than simply drinking milk or taking a calcium supplement. A diverse diet of natural foods that includes meat, fish, fresh vegetables, fruits and nuts will always cover the diverse nutritional needs of our bones as long as we stay away from high fat, high sugar and high sodium processed foods. Limit high fat protein sources, keep your salt intake low, reduce your alcohol consumption and don’t smoke and you’ll be fine. Also important is the amount of time spent outdoors. Get sunlight on your skin at safe times of the day for vitamin D as it plays an integral role in helping our body use calcium efficiently. As much as commercials warn us of the dangers of sunlight, recent studies have suggested that avoidance of sunlight is associated with higher risks of certain cancers- which should not be surprising as we did in fact evolve outdoors and not in the confines of fluorescent lit cubicles.
Dairy Products and Weight Gain

One of the most puzzling aspects of the practice of drinking milk and dairy products is that in a society where obesity is rampant, few are willing to give up what is essentially nature’s weight gain formula for young mammals. What puts that plump layer of fat on nursing babies and makes them expand almost as the days go by, is milk. From baby elephants to baby gorillas, milk is the primary food source when they are in early infancy and is responsible for a significant growth spike helping them to pack on. A mixture of water, sugars, fats and salt, milk is nature’s ultimate weight gain formula, helping infant mammals increase their body mass significantly in relatively short periods of time. Milk helps calves pack on hundreds of pounds to become cows, and interestingly enough, no adult mammal living in their environment consumes milk past infancy. Only humans and the animals we domesticate will drink milk as adults and it bears mentioning that the very countries with the highest dairy consumption are also the ones with the highest rates of obesity and metabolic disease. From a weight gain standpoint, as early as the 1950’s when bodybuilders wanted to decrease body fat and increase their muscular definition the first thing they would cut out of their diet was milk and dairy products as those were only consumed in the offseason when trying to get as big as possible. In the natural bodybuilding world today as well, dairy is almost universally restricted by those trying to reduce their body fat as it has been long observed that additions of seemingly benign products such as low fat yogurt make it more difficult to attain the higher degrees of muscle definition and lowered body fat needed for competitions. Whey protein shakes are also chucked aside during periods of contest dieting as they are in essence glorified milk shakes to say the least. (See my article on protein shakes and why you don’t need them here). Some studies, heavily popularized by the media found an association between dairy consumption and fat loss as the theory was that because dairy products contain calcium, protein and other bioactive compounds, that it might somehow favorably affect energy balance.[17] In randomized controlled trials, however these findings were inconsistent at best and a meta analysis of all the trials did not support the beneficial effect of increasing dairy consumption on body weight and fat loss in long-term studies or studies without energy restriction.[18] Finally, it is important to stress the role of exercise and not dairy intake as a way of increasing bone density. Weight training in particular plays a poignant role in maintaining and building healthy bone mass levels (Read my article here on weight training and osteoporosis). It’s a simple and scientifically proven way for prevention of low bone mass and in helping those with low bone mass levels build up their bones. So put down that glass of milk and start pumping some iron!
High Intensity Bodyweight Training: Ballistic Pushups & Dips!
This was a tough one!
Starts out with ballistic push ups (like clap pushups but without the clap as my wrist is still not 100%) nonstop for 20 reps, then all out on dips for 10 reps.
To say it was painful would be an understatement, but you just have to push through and keep on going.
Still training, hope you are too and as always, Excelsior!!! #naturallyintense
#hometraining #homeworkout #homeworkout #highintensitytraining #naturalbodybuilder #naturalbodybuilding #fitover40 #naturalbodybuildingvideos #chestday #chesttraining #naturalbodybuildingtips #pushups #dips #bodyweighttraining #highintensitytrainingtips #drugfreebodybuilding #calesthenics
Kevin's Unconventional Biceps Training- 3-6 Minutes a Week!
In this video I go over my biceps training using the Naturally Intense High Intensity Training protocols that helped me go from having arms measuring 11.5 to 12 inches to 18 inches drug free!
It's an unconventional approach for certain, but it's one that's helped my arms grow and the hundreds of men and women I have trained over the past 30 plus years.
Now, my success isn't due to being genetically gifted, as it took me the better part of 11 years to get my arms up to those measurements.
Which is significant as it works and been been proven time and time again to work for the average man or woman trying to grow their arms without drugs.
It's my hope that these high intensity training protocols can help you as much as they helped me!
Click on my bio link to see the full video on my YouTube channel and thanks as always for taking the time to look at my work!!! Excelsior!!! #naturallyintense
#highintensitytraining #naturalbodybuilder #naturalbodybuilding #fitover40 #naturalbodybuildingvideos #armworkout #bicepsworkout #naturalbodybuildingtips #biceps #armtraining #highintensitytrainingtips #drugfreebodybuilding #barbellcurls
At the Lancaster Classic Day 2 Elimination Rounds Against European Champion, and World Record Holder Leo Pettersen @leo_barebow_archer
I don't talk much about it but I'm also a competitive barebow archer (surprise!) and last Saturday I had the honor of making it to Day 2 at the Lancaster Archery Classic in the Barebow Division, as I made the top 64 out of 267 competitors and had a chance to shoot with some of the greatest barebow shooters on the planet!
I didn't make it past Leo, but it was a real rush to be there and a huge thanks to my coach, Joe MyGlyn @prolinearchery for helping me get there.
Thanks as well to my good friend @sean_chan33 for all of his help from the very start, to my line buddy Aaron Shea for taking the shot and showing up to support!
My thanks as well to rob_kaufhold for putting on and promoting one of the best archery tournaments on earth!
Thanks also to to everyone who took the time to send a supporting word and I am looking forward to next year!!! #naturallyintense #barebow
#lancasterclassic #lancasterarcheryclassic2024 #lancasterarchery #archery #fitover40 #barebowrecurve #targetarchery
Dumbo, Brooklyn circa 2004
This shot was taken as part of the promotion for my Naturally Intense DVD and was about a year after my last bodybuilding competition.
It was a grueling photoshoot.
We started at about 10 am and finished around 4pm and I was completely spent, but the more we shot the sharper I looked, so we kept on going.
It's nice to look back from time to time and as tired as I was, we all had a blast!
My thanks to @stephanie_corne_artwork, @https://pulse.ly/itgnag2dec and @ftaz1 for taking the shots!!!
Thanks for watching and as always, Excelsior!!! #naturallyintense
#naturalbodybuilder #naturalbodybuilding #throwback #fifthavenuegym #5thavenuegym #drugfreebodybuilding #naturalbodybuildinglifestyle #gymlife #gymmotivation #naturalbodybuildingmotivation #bodybuilding #blackandwhite #instablackandwhite #bnw
Can You Build An Impressive Physique Training Only At Home?
Absolutely!
I stopped training in commercial gyms as of March 2020 and have been training at home ever since.
Initially I was admittedly worried that I might lose some of my gains or not make as much progress, but that certainly wasn't the case.
I've consistently continued to improve with my high intensity workouts and muscles have no idea where they are training.
As long as the criteria of adequate intensity and overload are met, there will be an adaptive response and your muscles will get bigger and stronger.
So don't worry at all about where you train, focus instead of what will be the best way for you to always be training!
Thanks for watching and as always, Excelsior!!! #naturallyintense
Kevin's Three Day Training Spilt!
For the past 33 years I have trained three times a week with Naturally Intense High Intensity Training workouts lasting 10, 15 to 20 minutes max.
It's a training split tried and testes not only in it's helping me realize my goal of becoming a successful natural bodybuilder, but it's also helped hundreds of men and women over the past three decades.
I have tested just about every possible training split imaginable and for this particular style of high intensity training, this particular grouping consistently yields fantastic results.
I hope it helps you as much as it's helped me over the years and thanks so much for taking the time to look at my work.
Keep training hard and Excelsior!!! #naturallyintense
Excelsior!!! #naturallyintense
#trainingsplit #3daytrainingsplit #threedaytrainingsplit #naturalbodybuilding #naturalbodybuilder #naturalbodybuildingvideo #naturalbodybuildingmotivation #naturalbodybuildingtips #drugfreebodybuilding #bodybuilding #highintensitytraining #highintensitytrainingtips
405 Stiff Leg Deadlift for 7 Reps! High Intensity Training.
First leg workout of the year and already pushing it!
I haven't done a stiff leg deadlift over 315lbs for about 3 years at this point, and I did my last set with 315lbs and comfortably got to 10 reps and decided I had far too much gas left in the tank and that I should go up in weight.
So I did.
I figured I might get a solid 6 reps in, but I made it to 7 and I think I could have gone on to get a full 10 reps BUT that's when good judgement prevailed.
As a bodybuilder having not trained this heavy for so many years, the shock of this much weight would be more than enough to stimulate muscle growth, and doing more reps wouldn't yield any greater returns, only increase the likelihood of injury.
It's not about the numbers, it's about training to a point where you achieve your goal, and it's important to have a goal in mind as a bodybuilder based on increasing muscle mass rather than hitting a particular number.
Besides, if in my 20's I never did more than 405lbs on a stiff leg deadlift, it doesn't make any sense going heavier than when I am almost 50!
Could I deadlift more at this point?
Absolutely but just because you can doesn't mean you should!
So keep those weights in a good working range, keep it safe and as always Excelsior!!! #naturallyintense
#hometraining #homeworkout #homeworkout #roguerack #highintensitytraining #naturalbodybuilder #naturalbodybuilding #fitover40 #naturalbodybuildingvideos #backworkout #naturalbodybuildingtips #backtraining #highintensitytrainingtips #drugfreebodybuilding #fitoverforty #deadlift
Turning 50 in a few months...
Not much of a big deal for me as I still feel pretty much the same but I hope that my example helps show what can be done with a lifetime commitment to eating well and training consistently!
Thanks for coming along on the journey and as always, Excelsior!!! #naturallyintense
#naturalbodybuilder #naturalbodybuilding #healthylifestyle #fitover40 #drugfreebodybuilding #naturalbodybuildingmotivation #natty #fitness
Please note that all material is copyrighted and DMCA Protected and can be reprinted only with the expressed authorization of the author.

Click To Get A Copy Of Kevin’s Free Ebook On The Role Of Exercise In Reducing Abdominal Fat!
Featured everywhere from the Wall Street Journal to CBS News, Kevin Richardson is an award winning personal trainer, natural bodybuilding champion, creator of Naturally Intense High Intensity Personal Training and one of the best personal trainers in New York City.
If you liked this article you may also be interested in:
Related Articles:
How Weight Training Prevents Osteoporosis
References for Do You Need Milk For Strong Bones:
1. Xu L, Lu A, Zhao X, Chen X, Cummings SR.Very low rates of hip fracture in Beijing, People’s Republic of China the Beijing Osteoporosis Project. Department of Obstetrics and Gynecology, Peking Union Medical College Hospital, Beijing, People’s Republic of China. Am J Epidemiol. 1996
2. Cummings SR and Melton LJ. Epidemiology and outcomes of osteoporotic fractures. Lancet 2002
3. Kanis JA, Johnell O, De Laet C, et al. A meta-analysis of previous fracture and subsequent fracture risk. Bone 2004
4. Kanis JA and Johnell O. Requirements for DXA for the management of osteoporosis in Europe. Osteoporos Int 2005
5. Melton LJ, Cooper C. Magnitude and impact of osteoporosis and fractures. In: Marcus R, Feldman D, Kelsey J (eds.) Osteoporosis 2001
6. Gender and ethnic differences in intakes of dairy foods and related nutrients, obesity, and metabolic outcomes: NHANES, 1999–2004
7. Per Capita Consumption of Milk and Milk Products in Various Countries, International Dairy Federation, Bulletin 423/2007
8. Heaney, R.P., Evaluation of publicly available scientific evidence regarding certain nutrient-disease relationships 3. calcium and osteoporosism Life Science Research Office, Federation of American Societies for Experimental Biology, Bethesda, MD 1991
9. Wachman, A., et al. Diet and osteoporosis. Lancet May 4, 1968
10. Recker, R., The effect of milk supplements on calcium metabolism, bone metabolism, and calcium balance. American J Clin Nutr 1985
11. Nilas, L. Calcium supplementation and post menopausal bone loss. British Medical Journal 1984
12. Kolata, G. How important is dietary calcium in preventing osteoporosis? Science 1986
13 Institute of Medicine. Dietary reference intakes for calcium, phosphorus, magnesium, vitamin D, and fluoride. Washington, DC: National Academy Press, 1997.
14. Alaimo K, McDowell MA, Briefel RR, et al. US Department of Health and Human Services. Dietary intake of vitamins, minerals, and fiber of persons ages 2 months and over in the United States: third National Health and Nutrition Examination Survey, Phase 1, 1988–91. Hyattsville, MD: National Center for Health Statistics, 1994. (Advance data from vital and health statistics no. 258.)
15. Weaver CM, Plawecki KL. Dietary calcium: adequacy of a vegetarian diet. Am J Clin Nutr 1994
16. Dietary Supplement Fact Sheet. US Office of Dietary Supplements
17. Barr SI. Increased dairy product or calcium intake: is body weight or composition affected in humans? J Nutr 2003
18. Chen M, Pan A, Malik VS, Hu FB. Effects of dairy intake on body weight and fat: a meta-analysis of randomized controlled trials. The American Journal of Clinical Nutrition. 2012






